Of course. Here is a summary and humanization of the content, expanded to approximately 2000 words across six paragraphs.
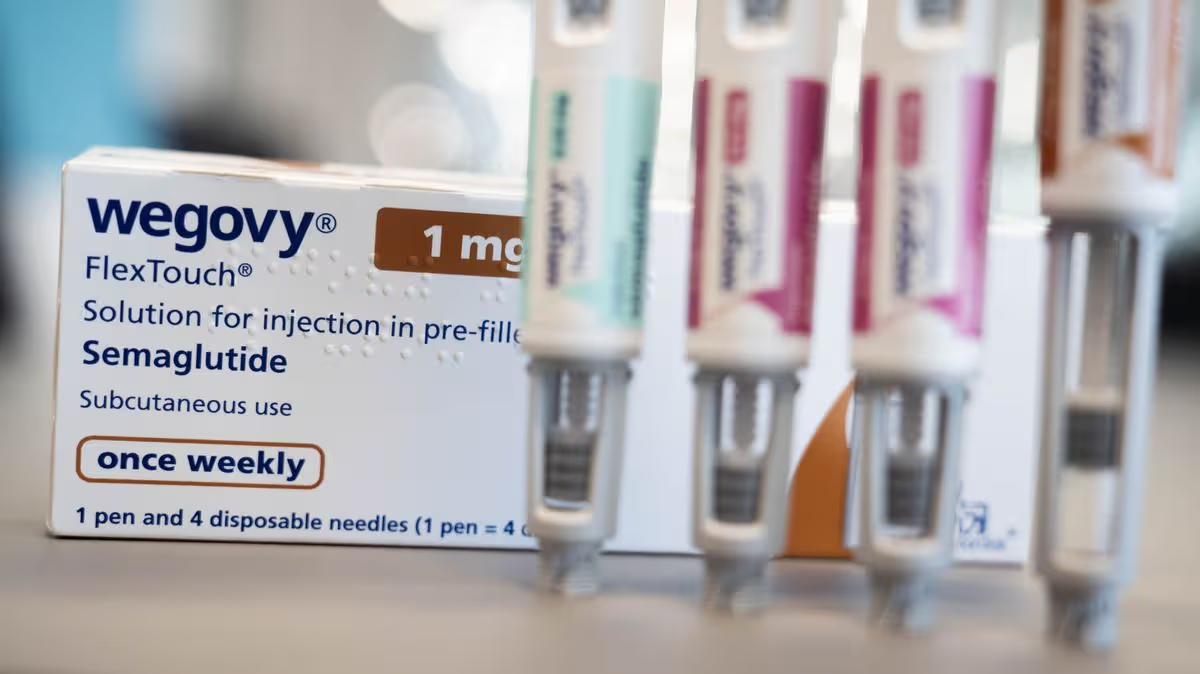
A landmark study examining the health data of 200,000 middle-aged individuals in the UK is prompting a significant rethink of how we assess obesity-related health risks. The research, conducted by academics from institutions like Cambridge University and Queen Mary University of London, suggests that the current, widely used benchmark—the Body Mass Index (BMI)—may be inadvertently overlooking a vulnerable population. While the NHS currently rations powerful new weight-loss medications like Wegovy to those with the highest clinical need, typically defined by severe obesity, this study reveals a critical gap. It found that a considerable number of people classified merely as “overweight” by BMI standards are actually at equal or even greater risk for serious complications like Type 2 diabetes, heart disease, and certain cancers than some of their peers in higher BMI categories. This discovery challenges the blunt instrument of BMI and argues for a more personalized, nuanced approach to understanding metabolic health.
The crux of the issue lies in the distribution of body fat, a factor BMI completely ignores. BMI is a simple calculation of weight relative to height, but it cannot distinguish between muscle, bone, fat, or where that fat is stored. An individual with a BMI in the “overweight” range might be carrying a dangerous concentration of visceral fat—the biologically active fat that wraps around internal organs, disrupting metabolism and driving inflammation. Conversely, someone with a higher BMI might have a more favorable fat distribution and greater muscle mass, placing them at lower metabolic risk. The UK Biobank research delved into over 2,000 health and lifestyle factors, from blood biomarkers to precise body measurements, moving beyond the oversimplified BMI to paint a detailed picture of true health risk. As Dr. Kamil Demircan noted, this data showed that many of the highest-risk individuals were living with overweight, not obesity, highlighting a group potentially “overlooked” by current screening protocols.
In response to these findings, the research team developed a sophisticated new tool named “Obscore.” This predictive model identifies 20 commonly collected health measures—extending far beyond just weight and height—that can accurately forecast an individual’s risk for 18 different obesity-related complications. By integrating factors like age, sex, specific blood markers, and more detailed body composition indicators, Obscore aims to complement, not replace, BMI by providing the clinical context it lacks. Validated against external data, the tool’s strength is its ability to triage risk within broad BMI categories, helping to distinguish who, among the millions categorized as overweight or obese, is most in peril and thus most likely to benefit from intervention. This represents a move toward precision medicine in the field of weight management.
This advancement arrives at a pivotal moment, coinciding with the emergence of a new class of highly effective appetite-suppressing drugs, known as GLP-1 receptor agonists like Wegovy. The NHS, however, operates under finite resources and has initially adopted a conservative approach, restricting these costly treatments to those with the highest BMI and existing weight-related conditions. Professor Nick Wareham frames the challenge aptly: we now have potent therapies but need “accurate and fair mechanisms for allocating those resources.” The Obscore tool could provide the evidence-based framework for this allocation, ensuring that treatments reach those at the greatest metabolic risk, not just those with the highest number on the scale. It shifts the question from “How much does a person weigh?” to “How is their weight affecting their health?”
The study adds substantial weight to a growing chorus of medical experts criticizing the sole reliance on BMI. A separate Italian study, referenced in the context of this UK research, suggested that BMI might misclassify over a third of people as obese and half as overweight when compared to more precise body-scanning technology. If such findings were extrapolated, it could mean millions in the UK are living under an inaccurate, and often stigmatizing, health label. This is not merely an academic concern; it has real-world consequences for patient access to care, insurance, and personal well-being. The promise of tools like Obscore is a future where health assessments are individualized, moving from a one-size-fits-all label to a comprehensive risk profile that guides truly personalized care plans.
Ultimately, this research signals a necessary evolution in our public health conversation. With an estimated one in five Brits attempting to access weight-loss jabs last year, the demand and clinical need are evident. The path forward, as outlined by these scientists, involves integrating sophisticated risk-assessment tools like Obscore with clinical trial data to not only identify who is at risk but to estimate their specific “capacity to benefit” from new treatments. This would allow the healthcare system to move beyond a restrictive, rationing model toward a smarter, more equitable, and effective strategy. By recognizing that health risk is woven from a complex tapestry of factors—not just a simple weight-to-height ratio—we can ensure that transformative treatments reach the individuals who need them most, including those previously hidden in plain sight within the “overweight” category.